Fluid Resuscitation | Vibepedia
Fluid resuscitation is the critical medical practice of restoring lost bodily fluids, a cornerstone of emergency and critical care. Whether due to hemorrhage…
Contents
Overview
Fluid resuscitation is the critical medical practice of restoring lost bodily fluids, a cornerstone of emergency and critical care. Whether due to hemorrhage, dehydration, sepsis, or burns, rapid and appropriate fluid administration can mean the difference between life and death. Historically, intravenous (IV) therapy has been the dominant method, delivering fluids directly into the bloodstream for rapid absorption. However, the field is constantly evolving, with ongoing debates about the optimal types of fluids (crystalloids vs. colloids), the precise volumes and rates of administration, and the potential for iatrogenic harm from fluid overload. From the urgent needs of trauma patients to the complex management of critically ill individuals in the intensive care unit, fluid resuscitation remains a dynamic and vital medical intervention.
🎵 Origins & History
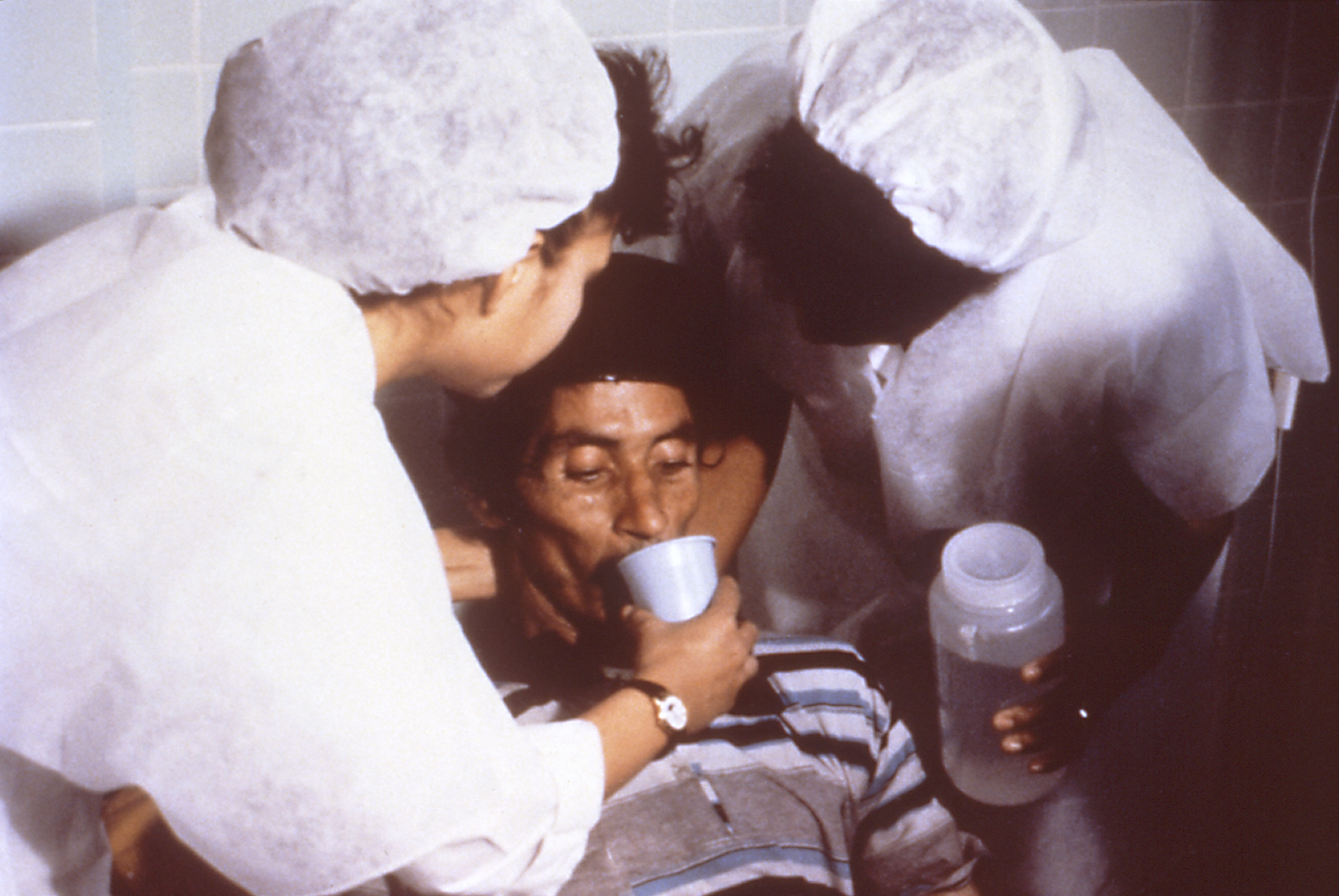
The concept of replacing lost bodily fluids dates back centuries, with early attempts involving oral or rectal administration. By the early 20th century, saline solutions were being widely used, particularly during World War I, to treat soldiers suffering from shock due to blood loss. Pioneers like George Crile championed the use of saline and William Halsted championed the use of blood transfusions, laying the groundwork for modern resuscitation protocols. The understanding of fluid dynamics and electrolyte balance, further elucidated by researchers like John Gibbon Jr. with his development of the heart-lung machine, continued to refine these practices.
⚙️ How It Works
Fluid resuscitation primarily involves administering intravenous fluids to restore circulating volume and maintain tissue perfusion. The body's fluid compartments are broadly divided into intracellular (within cells) and extracellular (outside cells), with the extracellular space further divided into interstitial (between cells) and intravascular (within blood vessels) spaces. When a patient loses significant fluid, particularly from the intravascular space due to bleeding or severe dehydration, their blood pressure drops, and vital organs become starved of oxygen. IV fluids, such as normal saline or Lactated Ringer's solution, are infused directly into the veins, rapidly expanding the intravascular volume. This increases venous return to the heart, boosts cardiac output, and consequently improves blood pressure and oxygen delivery to tissues. The choice of fluid and the rate of administration are tailored to the specific clinical scenario, balancing the need for volume expansion with the risk of fluid overload.
📊 Key Facts & Numbers
The Parkland formula is used to calculate fluid resuscitation requirements for severe burns. The global market for intravenous solutions alone is projected to exceed $15 billion by 2027, underscoring the sheer volume of fluids administered worldwide. Despite these volumes, up to 30% of critically ill patients may still develop signs of fluid overload, leading to complications like pulmonary edema.
👥 Key People & Organizations
Key figures in the development of fluid resuscitation include Christiaan Barnard, who performed the first human-to-human heart transplant and relied heavily on fluid management. William McCartney Potts was a pioneer in pediatric surgery, emphasizing careful fluid balance in young patients. Organizations like the Society of Critical Care Medicine and the American College of Surgeons play crucial roles in setting guidelines and disseminating best practices through initiatives like the Surviving Sepsis Campaign. The World Health Organization (WHO) also provides guidance on oral rehydration therapy, a vital form of fluid resuscitation for diarrheal diseases, particularly in low-resource settings. Research institutions like the Johns Hopkins University and Harvard Medical School continue to contribute significant research in this field.
🌍 Cultural Impact & Influence
Fluid resuscitation has profoundly shaped emergency medicine, trauma care, and intensive care. The ability to rapidly reverse shock states has transformed outcomes for countless patients who would have previously succumbed to their injuries or illnesses. It's a visible intervention, with IV bags and lines becoming iconic symbols of critical care in media portrayals, from battlefield dramas to hospital procedurals. The principles of fluid management extend beyond acute care, influencing post-operative recovery and the management of chronic conditions. The widespread availability of IV fluids has also democratized critical care, making advanced resuscitation techniques accessible in diverse settings, though disparities in access remain a significant global challenge. The development of specialized fluid formulations, like hydroxyethyl starch (though now largely restricted due to adverse effects), also reflects the ongoing quest for more effective resuscitation agents.
⚡ Current State & Latest Developments
Current trends in fluid resuscitation focus on personalized medicine and minimizing fluid overload. Advanced monitoring techniques, including echocardiography, pulse-contour analysis, and passive leg raising maneuvers, are increasingly used to guide fluid decisions. There's also a growing interest in the use of balanced crystalloids, such as Plasmalyte, over normal saline, due to concerns about saline's potential to cause hyperchloremic acidosis. Research is also exploring novel resuscitation fluids and adjunct therapies to improve oxygen delivery and reduce organ damage.
🤔 Controversies & Debates
One of the most persistent controversies in fluid resuscitation is the crystalloid versus colloid debate. While crystalloids like saline are inexpensive and readily available, they distribute more widely into the interstitial space, potentially leading to peripheral edema. Colloids, such as albumin or hydroxyethyl starch, are thought to remain in the intravascular space longer, theoretically providing better volume expansion. However, concerns about the safety and efficacy of colloids, particularly hydroxyethyl starch's association with kidney injury and coagulopathy, have led many guidelines to favor crystalloids. Another major debate centers on the optimal amount of fluid: too little can lead to inadequate perfusion, while too much can cause pulmonary edema, organ dysfunction, and increased mortality. The concept of 'permissive hypotension' in certain hemorrhagic shock scenarios, where blood pressure is intentionally kept lower to avoid dislodging clots, also remains a point of discussion.
🔮 Future Outlook & Predictions
The future of fluid resuscitation likely lies in even more precise, individualized approaches. Expect to see wider adoption of advanced hemodynamic monitoring integrated with artificial intelligence to predict fluid responsiveness and guide therapy in real-time. Research into novel fluid formulations with improved oncotic properties and reduced side effects will continue. Furthermore, a greater emphasis will be placed on understanding the 'why' behind fluid overload, exploring its impact on cellular function and immune responses. The integration of point-of-care diagnostics to assess tissue perfusion and organ function will become standard, allowing clinicians to tailor fluid therapy not just to blood pressure, but to actual physiological needs. The development of 'smart fluids' that can actively target areas of injury or inflammation is also a theoretical, albeit distant, possibility.
💡 Practical Applications
Fluid resuscitation is a fundamental intervention across numerous medical specialties. In emergency medicine and trauma care, it's used to manage shock from bleeding, burns, and dehydration. In critical care, it's essential for patients with sepsis, acute kidney injury, and pancreatitis. Anesthesiology relies on careful fluid management to maintain hemody
Key Facts
- Category
- science
- Type
- topic